Table of Contents
- How SARS-CoV-2 Is Detected
- What Is a Clinical Diagnostic Assay?
- A Closer Look at the SARS-CoV-2 Assay
- Ruling Out Possibilities When Testing for Coronavirus
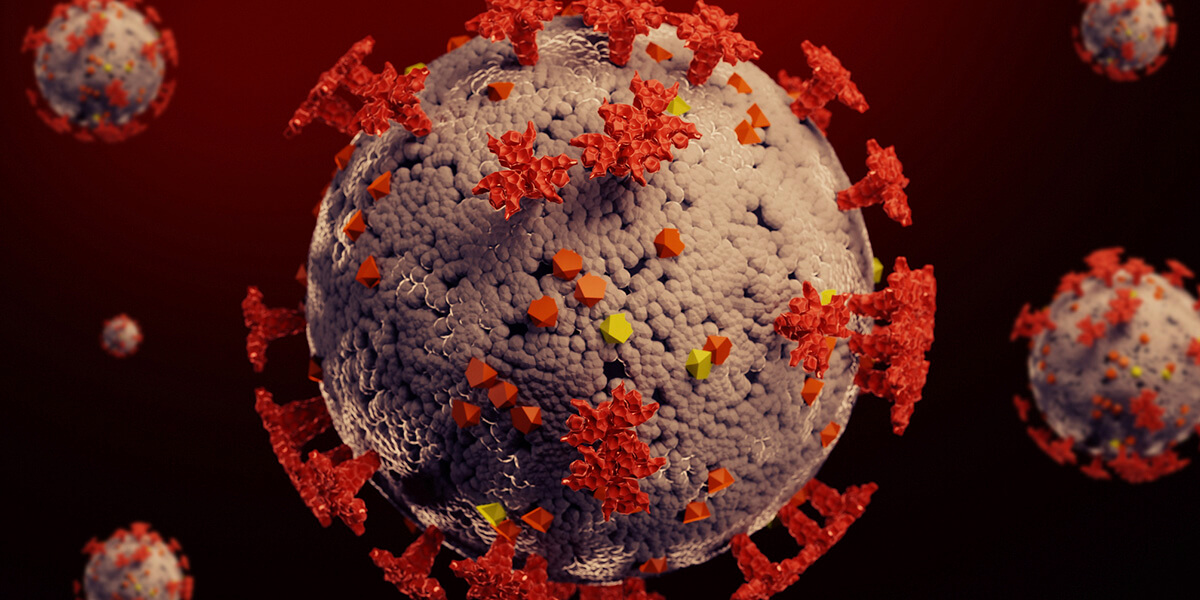
SARS-CoV-2 is a type of coronavirus that causes COVID-19. Before SARS-CoV-2, there were other coronaviruses like SARS-CoV and MERS-CoV, but SARS-CoV-2 is responsible for the pandemic that began in late 2019.
Coronavirus is named for its crown-like shape. This RNA virus is enveloped, non-segmented, and single-stranded, and it mostly affects animals. Six strains of the virus have affected humans, and many of them are responsible for a percentage of common colds. SARS and MERS are two examples of coronavirus that typically present with dire clinical features and a high infection rate, but SARS-CoV-2 brought about the largest spread of the virus.
In December 2019, a group of patients in Wuhan, China, were reported to the World Health Organization (WHO) for pneumonia with an unknown cause. By early January 2020, a full genome of the novel coronavirus had been sequenced.
Since the pandemic, SARS-CoV-2 assays have become one of the key testing methods for identifying the virus and preventing the spread of COVID-19. Learn how these coronavirus assays work and why they continue to be a trusted method for diagnosis.
Learn More About SARS-CoV-2 Assays
How SARS-CoV-2 Is Detected
Detecting SARS-CoV-2 with accuracy is critical for preventing the spread of the virus. Throughout the course of the pandemic, we’ve relied on various testing methods to diagnose patients with COVID-19. These tests use different methods to identify the presence of the virus, and the use of each testing method depends on circumstances and accessibility.
Molecular Test
Molecular tests look for target sequences in the DNA associated with SARS-CoV-2. There are a few types of molecular tests used to detect coronavirus. The most popular is the reverse transcription polymerase chain reaction (RT-PCR) test that isolates target sections of DNA and amplifies them.
While PCR tests are still among the most common molecular tests for detecting coronavirus, others include:
- Isothermal nucleic acid amplification: This testing method is still under development, but it can be performed at a fixed temperature — unlike the PCR. Rather than using these high temperatures to isolate target DNA strands, it uses DNA polymerases that can displace or “unzip” DNA as they synthesize other strands.
- CRISPR: Clustered regularly interspaced short palindromic repeats (CRISPR) is a newer method in coronavirus testing. This approach uses CRISPR RNA to cut a target region of a DNA strand. With the right detection signals, like fluorescence, the isolated region can be identified as positive or negative for coronavirus.
Antigen and Antibody Tests
These diagnostic tests can identify the presence of antibodies and antigens in the blood to prove the presence of SARS-CoV-2. Based on various studies, researchers have uncovered the genetic makeup of antibodies and antigens that are created to combat the virus. Antigen tests are valuable because they can detect mutations of the virus.
Antigen tests are immunoassays that detect the presence of a specific viral antigen, which indicates current viral infection. The performance of some of the antigen tests may not be impacted by mutations in the SARS-CoV-2.
CT Scan
With a computed tomography (CT) scan, physicians can analyze chest X-rays to find abnormal features that point to a diagnosis. This method is non-invasive, but the ability to detect the virus depends on the stage of infection. Lung characteristics generally have four phases throughout the infection, and different features manifest in the lungs within each stage.
What Is a Clinical Diagnostic Assay?
Diagnostic assays are used in life sciences or in the clinical science industry to analyze specific biological markers for clinical diagnostics or monitoring of risk factors.
Hospitals and labs use clinical diagnostic assays to determine whether a clinical sample contains a target analyte(s). Assay kits can measure the quantity or functional activity of the assay target or entity, which can be any of the following:
- Drug
- Compound
- Chemical element
- Organic sample
- Cell in an organism
- Microbial pathogen
Diagnostic tests enable healthcare professionals to diagnose diseases and monitor risk factors. With a clear understanding of the biological targets at work, providers can develop effective treatments for individual patients.
Reagents can be any chemical, process, or compound that can create a recognizable reaction with the target analyte. Clinical diagnostic assays can be used for a broad range of detection needs, including respiratory viruses, like SARS-CoV-2, gastrointestinal pathogens, and blood pathogens.
A Closer Look at the SARS-CoV-2 Assay
RT-PCR tests are an example of a clinical diagnostic assay. In this test, a healthcare provider collects a sample from the patient via nasal swab, throat swab, or saliva sample.
The sample goes into a testing machine that cycles through high and low temperatures that trigger reactions. These reactions lead to identical copies of target sections of DNA that are characteristic of SARS-CoV-2. A fluorescent dye is added to these DNA strands, and the computer will measure the level of fluorescence from each copied strand. When the fluorescence reaches a certain level, coronavirus is confirmed in the sample.
Coronavirus assays can be one-step or two-step tests. In a one-step PCR, only one tube with one sample is tested. Two-step PCR tests involve multiple tubes, which offers greater flexibility, but comes with the risk of cross-contamination. Automated systems are resolving this issue for more efficient testing.
RT-PCR assays can vary based on the manufacturer, especially when considering the system that triggers the reactions in the sample. At Applied BioCode Inc., our SARS-CoV-2 Assay detects two different genes related to the virus. This assay uses conjugated biotin primers and BMB labeled probes to perform PCR first, then in the presence of SA-PE, signals are detected. It will not detect other common coronavirus genes to deliver more focused results.
The BioCode® SARS-CoV-2 Assay has an Emergency Use Authorization (EUA) from the Food and Drug Administration (FDA) for use by laboratories certified under the Clinical Laboratory Improvement Amendments (CLIA) of 1988. It is not FDA-cleared or approved.
These assays work with our BioCode® MDx-3000 system which supports processing 96 samples and is ideal for high throughput testing. With our system, healthcare professionals can run up to three different panels at once for greater efficiency. Our system validates DNA extraction to confirm the validity of your sample and automates the target detection and capturing process. With clear reporting following the test, users can be sure when a result is positive or negative.
Ruling Out Possibilities When Testing for Coronavirus
One of the early challenges with diagnosing COVID-19 was the similarities the illness had to other respiratory diseases. SARS-CoV-2 assays are an ideal way to identify the presence of the virus in a given sample, but testing for all possible respiratory illnesses for a set of clinical manifestations is recommended.
The BioCode® CoV-2 Flu Plus Assay is a multiplex assay with an EUA from the FDA that tests for the presence of SARS-CoV-2, Influenza A, Influenza B, and Respiratory Syncytial Virus (RSV). Since these four viruses have similar clinical presentations, our multiplex assay can give direct answers regarding infection without needing to use multiple tests. The CDC supports the use of these multiplex assays.
If these four targets come back negative following a multiplex assay, you can run our Respiratory Pathogen Panel to detect and differentiate between 17 respiratory viruses.

Learn About the SARS-CoV-2 Multiplex Assays From Applied BioCode Inc.
SARS-CoV-2 is a virus with a high infection rate, so confirming positive infections is critical to protecting public health. At Applied BioCode Inc., our SARS-CoV-2 assay and multiplex assay products are the keys to accurate diagnoses when working with patients who may have COVID-19. Use our system and assay kits to rule out diagnoses and guide treatment to prevent the spread of coronavirus within populations.
Get in touch with us today to learn more about our assay kits.